Understand when diarrhea in a child becomes dangerous. Learn the warning signs of dehydration, high fever, blood in the stool, and when medical attention is necessary.

Acute diarrhea in children most often follows a mild and self-limiting course. However, the question of when diarrhea in a child is dangerous is entirely justified. The severity of the condition is not determined by the number of bowel movements, but rather by the child’s overall condition, the degree of dehydration, and the presence of additional warning symptoms. These factors determine whether further medical evaluation or hospital treatment is required.
Assessment of Dehydration
The most significant risk associated with diarrhea is the loss of fluids and electrolytes. A child’s body, particularly in infancy, has limited compensatory mechanisms, and clinical deterioration may occur rapidly. Early signs of dehydration include dry lips and oral mucosa, reduced urination, and increased thirst. Parents often notice behavioral changes — the child may become quieter, more irritable, or unusually fatigued.
As dehydration progresses, more pronounced clinical signs may appear, such as sunken eyes, decreased skin elasticity, cold extremities, and drowsiness. In advanced stages, the child may be difficult to awaken, apathetic, or cry without tears. These are signs of significant fluid loss and require immediate medical attention. A detailed description of the degrees of dehydration can be found in the separate article dedicated to the topic.

General Condition – The Most Reliable Indicator
In clinical practice, a child’s general condition is more important than the frequency of bowel movements. If the child remains active and continues to drink fluids adequately, the illness is usually mild. In contrast, marked lethargy, lack of interest in surroundings, or difficulty awakening are concerning signs.
A sudden behavioral change is often the first indication of complications. In young children, this may be the only early sign of clinically significant dehydration. Parental judgment plays a crucial role at this stage.
Blood in the Stool
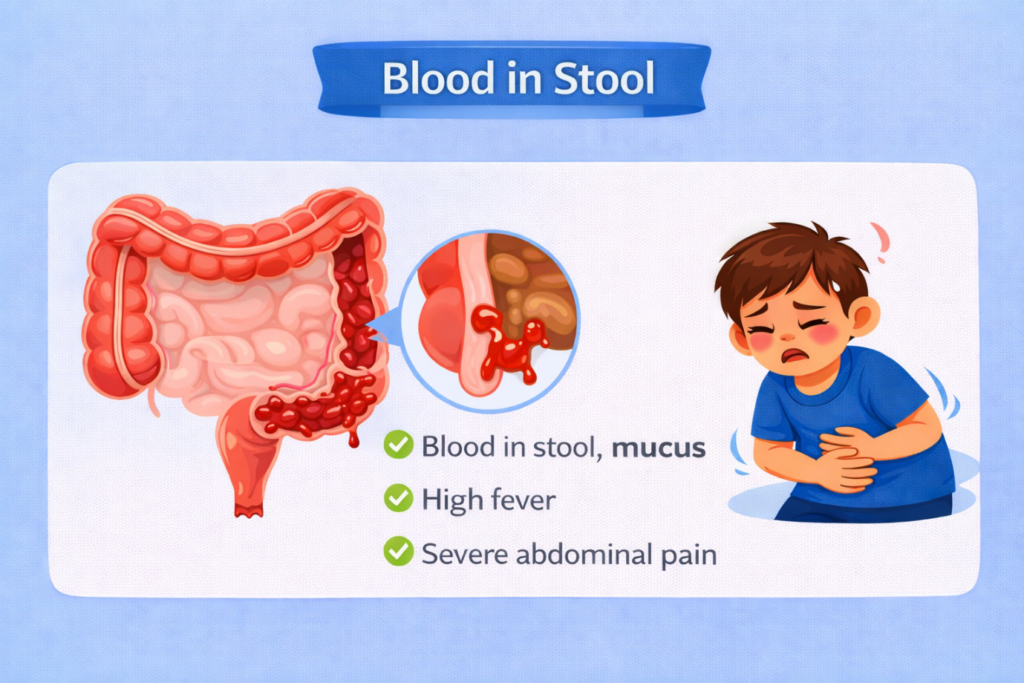
The presence of blood in the stool always requires medical consultation. Even small amounts suggest an inflammatory process involving the intestinal lining and are not typical of uncomplicated viral gastroenteritis. In many cases, the cause is a bacterial infection with invasive involvement of the intestines.
Blood may appear as bright red streaks on the surface of the stool or be mixed within it. It may also be accompanied by mucus, high fever, and significant abdominal pain, increasing the likelihood of inflammatory colitis.
It is important to distinguish true intestinal bleeding from small streaks of blood caused by anal fissures due to frequent bowel movements. However, this distinction should not rely solely on parental description — medical evaluation is necessary. Blood in the stool, especially when accompanied by deterioration in general condition, requires further assessment and possible laboratory testing.
Abdominal Pain
Mild, diffuse abdominal pain commonly accompanies viral gastroenteritis and is usually transient, with fluctuating intensity and improvement after bowel movements. It is typically colicky in nature, occurring in waves, and the child remains relatively well between episodes.
Persistent, worsening, or clearly localized abdominal pain requires closer evaluation. Pain that does not improve after defecation or intensifies over time necessitates differential diagnosis. Particular attention should be paid to pain in the right lower abdomen.
In clinical practice, surgical conditions such as appendicitis, intussusception, or other acute abdominal processes must be excluded, especially when pain is accompanied by vomiting, high fever, or progressive lethargy. In infants, sudden intense crying, pulling the legs toward the abdomen, or alternating irritability and apathy may indicate a more serious condition.
Duration and Symptom Dynamics
The duration of diarrhea must be interpreted within the context of symptom progression. Typically, acute viral diarrhea peaks during the first few days and gradually improves. If there is no clinical improvement after the first week — or if symptoms worsen — further evaluation is necessary.
Persistent diarrhea lasting more than two weeks requires a more in-depth diagnostic approach. Possible causes include ongoing infection, post-infectious lactose intolerance, disruption of the intestinal barrier, or other underlying conditions.
Special attention should be given to cases involving progressive weight loss, poor appetite, or failure to thrive in infants. Recurrent episodes within a short period should also be carefully assessed.
Vomiting and Inability to Maintain Oral Intake
Frequent vomiting significantly increases the risk of dehydration, especially when combined with diarrhea. While isolated vomiting episodes may accompany infection, repeated vomiting that prevents fluid retention substantially changes the clinical picture.
In such cases, the child loses the ability to maintain effective oral hydration, and the risk of rapid deterioration increases. Prolonged vomiting may also lead to electrolyte imbalances.
If the child becomes progressively lethargic, urinates infrequently, or cannot tolerate even small amounts of fluids, hospital evaluation and intravenous rehydration may be necessary.

High Fever and Systemic Symptoms
Fever commonly accompanies acute gastroenteritis and does not automatically indicate severe illness. However, diarrhea becomes more concerning when the fever is high, persistent, or accompanied by worsening general condition.
A temperature above 38.5–39°C (101.3–102.2°F) lasting more than two to three days — particularly when combined with pronounced fatigue, severe abdominal pain, or blood in the stool — may suggest bacterial infection or complications.
In infants and young children, high fever may be the only early indicator of a more serious condition. Fever that does not respond to antipyretics, is accompanied by chills, or makes the child appear toxic requires prompt medical evaluation.
High-Risk Groups Requiring Lower Threshold for Evaluation
Certain groups of children should always be examined more promptly. These include infants under three months of age, premature babies, and children with chronic medical conditions. In these cases, dehydration can develop more rapidly and clinical signs may be subtle.
Children with immunodeficiency or those receiving immunosuppressive therapy are at increased risk of prolonged or complicated illness. The same applies to patients who have recently received antibiotics, due to the risk of antibiotic-associated diarrhea.
Early assessment in these groups allows timely intervention and prevention of complications.
When Is Diarrhea in a Child Dangerous and Requires Emergency Care?
Diarrhea in a child is dangerous when accompanied by signs of severe dehydration, blood in the stool, intense abdominal pain, high fever with poor general condition, or altered consciousness.
In these situations, home monitoring is insufficient, and urgent medical evaluation or hospitalization may be necessary.
In summary, severity is determined not by the number of bowel movements, but by the overall clinical picture. Monitoring behavior, fluid intake, and early signs of dehydration remains essential. When in doubt about whether diarrhea is dangerous, timely medical consultation is always the safer approach.
Important Disclaimer
The information in this article is for educational and informational purposes only. It does not replace medical examination, diagnosis, or personalized consultation with a healthcare professional. If symptoms persist, signs of dehydration develop, fever remains high, blood appears in the stool, or the child’s condition worsens, prompt medical evaluation is required.
Dr. Angel Todev
Infectious Diseases Specialist
